Unless you belong to the 10-15% of people that have gallstones, you probably never think about your gallbladder or its function. However, this small pear-shaped organ plays an important role in our digestive system. The gallbladder is situated right under the liver, and stores bile produced by liver cells. Mostly after eating meals, bile is released from the gallbladder into the gut. Here, substances within the bile called bile acids help with the breakdown and absorption of fat. Apart from their role in the digestive system, bile acids have been shown to communicate with other organs and thereby affect the metabolism of fat and sugar. Not unexpectedly, considering their roles in digestion and metabolism, bile acids are associated with various metabolic diseases in humans, such as obesity and diabetes. Modulation of bile acids could therefore be used as a strategy to treat or prevent such metabolic disorders.
Dr. Antwi-Boasiako Oteng and colleagues from the Haeusler lab of the Department of Pathology & Cell Biology at Columbia University aimed to better understand how bile acids influence metabolic health. The two primary bile acids in humans are cholic acid (CA) and chenodeoxycholic acid (CDCA), which are both made from cholesterol in the liver (see Figure below, left panel). CA production requires the enzyme Cyp8b1, which adds a hydroxyl group (i.e., one hydrogen atom bonded to one oxygen atom) to the 12th carbon of the molecule. Because of this modification, CA is called a “12α-hydroxylated bile acid”. CDCA does not contain this hydroxyl group on its 12th carbon, and is therefore called a “non-12α-hydroxylated bile acid”. Levels of 12α-hydroxylated bile acids like CA are higher in obese individuals, but it is not yet known whether they can cause obesity. Therefore, in their study published in Molecular Metabolism, the researchers investigated the role of non-12α-hydroxylated versus 12α-hydroxylated bile acids in the development of metabolic disorders in an experimental mouse model.
Dr. Oteng and colleagues started their research by genetically manipulating mice in such a way that they have bile acids more similar to humans. This is necessary as mice produce bile acids called muricholic acids (MCAs) that are not present in humans. By removing the enzyme that converts CDCA into MCA, the researchers created mice with a human-like bile acid profile (see Figure below, right panel). Aside from having low levels of MCA, these mice had higher levels of CDCA and lower levels of CA as compared to regular mice. Most importantly, fat absorption was strongly reduced in these mice, and they were protected from weight gain when fed a high-fat diet. To test if this could be due to the relative decrease in 12α-hydroxylated bile acids, the researchers supplemented another group of human-like mice with high levels of 12α-hydroxylated bile acids. This treatment strongly promoted fat absorption, which may increase susceptibility to metabolic disorders when combined with an excessive and/or unhealthy diet.
These findings suggest that the ratio of non-12α-hydroxylated versus 12α-hydroxylated bile acids is an important determinant of metabolic health in humans, which opens up new avenues for therapeutic intervention. According to Dr. Oteng, “We now have increased confidence that targeting Cyp8b1 to reduce the levels of 12α-hydroxylated bile acids can reduce the risk of metabolic disease in humans”. Currently, more than one-third of Americans have metabolic disorders, which increases their risk of heart disease and other health problems. If proven effective, a therapy targeting human bile acid composition could have a major impact on public health.
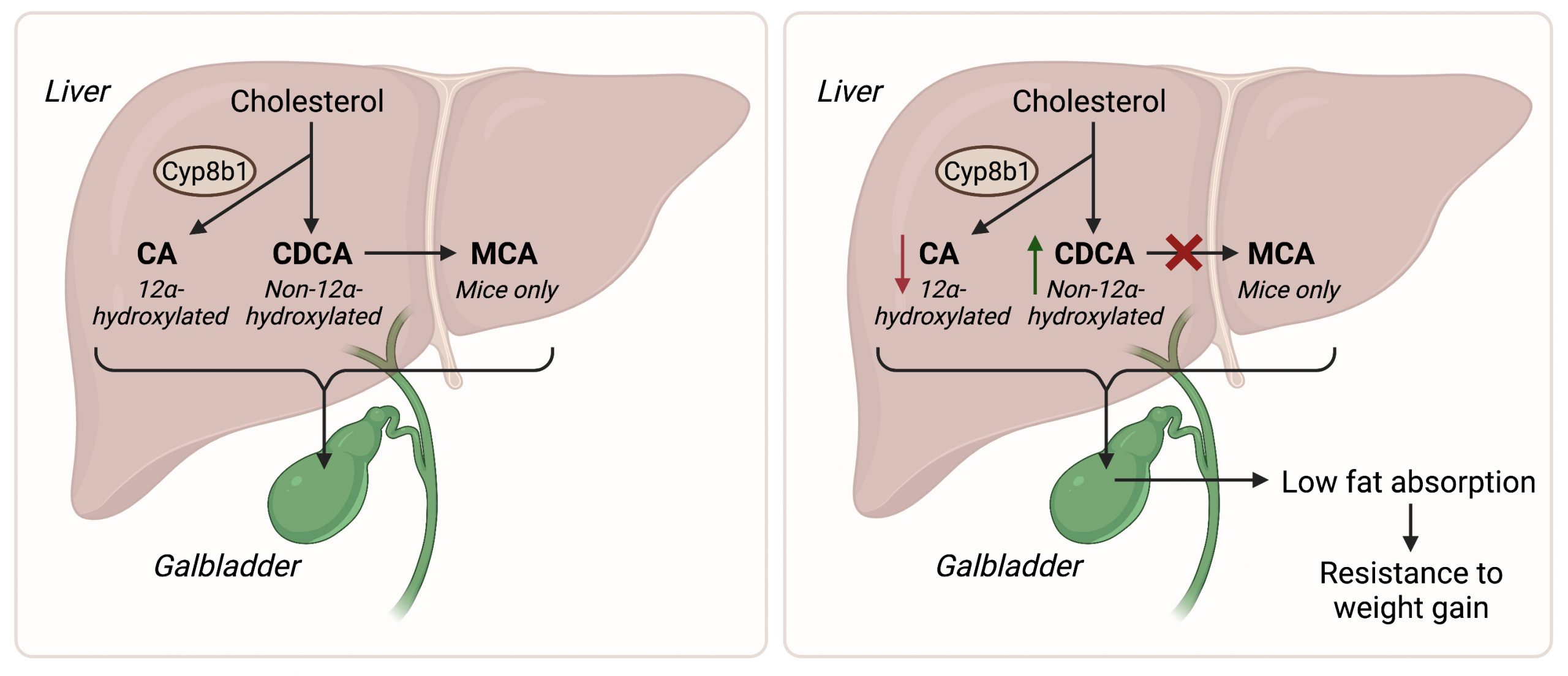
Left panel. The bile acids CA and CDCA are made from cholesterol in the liver. CA is 12α-hydroxylated bile acid produced by the enzyme Cyp8b1, while CDCA is non-12α-hydroxylated. In mice, CDCA is further converted into MCA. Right panel. Inhibition of the conversion of CDCA into MCA increases the ratio of non-12α-hydroxylated versus 12α-hydroxylated bile acids, thereby reducing fat absorption in the gut and protecting from diet-induced weight gain.